At a virtual town hall on Aug. 11, leaders from the county discussed monkeypox, its risks, and the County’s response to the local health emergency declared on Aug.2, a day after Gov. Gavin Newsom declared a state of emergency to respond to the monkeypox outbreak. San Diego County Chief Medical Officer Eric McDonald moderated the town hall with county experts, and with special messages from San Diego Mayor Todd Gloria, San Diego County Board of Supervisors Chair Nathan Fletcher, and District 3 San Diego Council member Stephen Whitburn.
County of San Diego Health and Human Services Agency Director Nick Macchione said the expert team was joined by members of the LGBTQ+ community who have been important partners in the county’s monkeypox response. “The county is taking our monkeypox response very seriously,” he said. “As our doctors, public health experts, and community leaders, we have been tracking monkeypox and ramping up our response to meet the needs for months. As an agency, we have a very robust infrastructure to respond to emerging health issues. Many of us have helped shepherd through many county health emergencies. I started my career 30 years ago with the emergence of HIV/AIDS pandemic.”
Macchione said that the county had a robust response to the COVID-19 pandemic, and though monkeypox is fundamentally different than COVID, it is important to know the county has “sharpened its ability” to address health emergencies through the years with COVID to create meaningful community partnerships.
Fletcher said it is imperative that accurate information is being shared about monkeypox, and the details about vaccines, prevention, and education.
“The county of San Diego has taken monkeypox very seriously, starting our response at the end of May when we been coordinating with our local healthcare partners,” he said. “We began an active information campaign. We held vaccination events with more coming once we get more vaccines for which we are continuously pushing. We distributed treatment courses to local hospitals and clinics.”
County Public Health Officer Dr. Wilma Wooten said the first monkeypox case was found in Massachusetts on May 17 and PHS set up its incident command structure on May 20. The first case in California was reported on May 27, with the first two probable cases in San Diego County reported on June 15. “This current outbreak is being seen in gay/bisexual, and men who have sex with men in our population,” she said. “Globally as of Aug. 6, CDC reported 3,800 cases in about 89 countries.
There are currently 9,482 confirmed cases in the U.S., and 1,310 confirmed and probable cases in the state of California. Locally, as of today we have 129 cases [updated through Aug. 11, there are 135 confirmed and probable cases], 17 more cases than reported yesterday. In the last demographics report on Aug. 8, with 104 cases, all were male. There have been no female cases to date.”
Wooten said the county started an active information campaign, including launching the County’s monkeypox website, a text monkeypox update, using social media platforms, LGBT media networks, Google, and launched a LGBT media campaign to promote monkeypox awareness and resources to the LGBT community through targets apps and websites.
County Deputy Health Officer Dr. Ankita Kadakia said monkeypox is a rare disease normally found in west and central Africa.
“This outbreak is unusual because of the large number of infections seen outside of Africa where it is pandemic,” she said. “Normally this is an infection that occurs inside of animals that can then pass infection to humans, but the current outbreak is person to person spread. The virus normally spreads through prolonged skin to skin contact, large droplet secretions in close face to face contact, and sharing contaminated towels, bedding or utensils. Monkeypox is harder to transmit than other infections like COVID-19, and although it can occur in any population, the risk to the general public is low, but there are certain groups that should take extra precautions.”
Kadakia said currently it is growing in the male to male sex population, but other groups such as children, pregnant women and the immune compromised should take precautions. She said the time from infection to symptoms is typically seven to 14 days from exposure but can range from five to 21 days and the illness can take from two to four weeks.
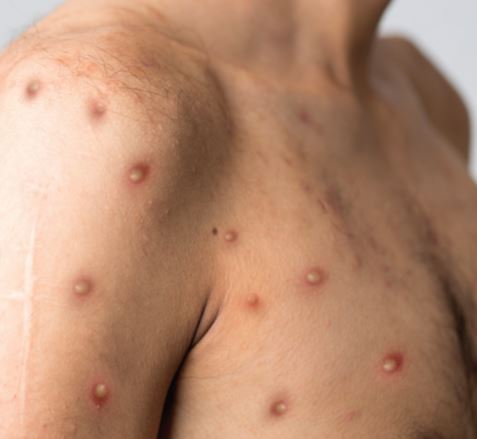
Kadakia said the rash typically begins on the face, to the palms and soles, and then the trunk, however, in this current outbreak rash has appeared in the genital areas, anal areas first, then oral lesions.
“We have requested 26,638 doses of the vaccine and we have received 5,047 doses from the California Department of Health, and 4,647 doses have been distributed, of which 2,377 have been administered. There are currently 400 doses reserved for post-exposure prophylaxis (PEP), she said. PHS HIV and STD and Hepatitis Branch Chief Patrick Loose said there are risks and practices that can on how people can reduce infection, especially in the gay/bisexual community.
“The vaccine supply right now is very limited, so we need to talk about the risk until the vaccine becomes more widely available,” he said. “These are the sex practices that can put you at greater risk for monkeypox. Oral sex, anal sex, vaginal sex, kissing, hugging and cuddling without clothes, and sharing sex toys.”
“Oral sex and anal sex in particular are the sex acts associated with monkeypox infection,” he said. “The reason for this is that they both involve prolonged skin to skin contact. Kissing also increases the risk of transmission. If someone is infected and has sores in their mouth or throat, they can secrete monkeypox virus in respiratory droplets and in saliva.”
Loose said prevention tips are to reduce the number of sex partners, reduce or avoid anonymous sex encounters, avoid group sex spaces, talk to your sex partners, and use condoms. He said how monkeypox is being transmitted now is not how it has been seen transmitted in the past.
“We do not know if people are infectious prior to showing symptoms,” he said. “We do know that monkeypox virus is found in semen. We do not know if it is found in vaginal secretion, feces, or urine. And we do not know the presence of monkeypox virus in semen can likely lead to transmission.” Public Health Services HIV, STD and Hepatitis Brand Medical Director Winston Tilghman said if you are diagnosed with monkeypox you may be contacted by the County who will ask about your sex partners and other close contacts so that they may be contacted about their exposure.
“We will do this anonymously, meaning we will not tell your recent partners who gave us their name and will connect them to needed resources, including testing and treatment or PEP,” he said.
San Diego County PHS San Diego HIV Planning Group Chair Mikie Lochner is a 36 longtime HIV/AIDS survivor and said he was thankful that county leaders jumped on this issue quickly.
“It has been a long two years with COVID-19, which is still here, and now monkeypox,” he said. “People are tired, scared, and even angry. And that is okay.” McDonald said that the number one question was why it was so hard to find a healthcare provider that can provide the vaccine. “The number of doses that we requested is about a quarter of what we might need,’ he said. “Much of that is committed to those who have been exposed. So, the supply is much lower than the demand, so we have had to actually prioritize them. We are not giving vaccines on demand but giving them on risks.”
McDonald said the White House announced on Aug. 9, the dosing scheme of one-fifth of a dose to be given between the folds of the skin intradermally which might quintuple the amount of vaccine available. Wooten said the County is supporting this strategy, extending a one vial does to five doses.
“We are planning a training effort to support this change to vaccine administration strategy,” she said.
Another question was why monkeypox is spreading now, has it mutated, and if it is more infectious.
Kadakia said the reason for the spread is person to person contact, and it is yet to be determined if the current strain is more infectious, but it does mutate, but not at the same rate as seen with COVID-19 and multiple variants.
Wooten said those who were old enough to have been vaccinated for smallpox, or vaccinated in the military, they are somewhat protected, but Kadakia said if you have not been vaccinated in the past three years, it is advised that you get the vaccine when available. Lochner said this is a skin to skin contact infection and is not a sexual transmitted disease.
“We need to get that message out to the entire community,” he said. “I would encourage all members of the community to learn how to protect yourself and your loved ones. This is for everybody. It is not just a one thing like the early years of the AIDS, where it felt like a certain portion of the community was being ostracized because it was a ‘gay disease.’ It is not a gay disease. Monkeypox can affect anybody. It does not discriminate.”
McDonald said when one part of the community is affected, it can potentially infect anybody and that everybody should be concerned. Wooten said in order to get tested for monkeypox, you must have the rash,
“Having those blisters is necessary to confirm the diagnosis,” she said.
For more information visit the County’s monkeypox web page, or text COSD MONKEY