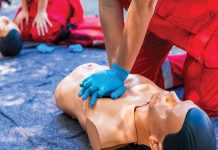
Now, 20 months after the first case of COVID-19 was confirmed in the U.S., there is evidence that people suffer from various conditions after having COVID and complaining of a multitude of symptoms and conditions.
With most, these conditions go away quickly, and people recover completely. But as the pandemic goes on, health professionals are seeing a large group of people that deal with symptoms and conditions, long after their bout with COVID. This group of people have been identified as “long haulers,” or those that are experiencing post COVID syndrome.
Dr. Kaveh Bagheri is board certified in internal medicine, and a pulmonologist, and critical care specialist, and has worked at Sharp Grossmont Hospital for the past 28 years.
In addition to his work at Grossmont, he has an outpatient pulmonary clinic for people who may not have access to providers due to lack of insurance or other reasons. He said the timing of the clinic was perfect as one of the services it now provides is care of patients with post-COVID conditions.
Bagheri said when physicians first started seeing COVID patients in the hospital, the only experience that they had came from literature about how China was experiencing the virus.
“We got hit hard in San Diego, just like the rest of the country,” he said. “Many of them died. Many of them did well and went home. Months later, many of us began seeing these patients coming to outpatient practices with many problems since they had COVID. That is where the term post-COVID condition was introduced. There are many terms for post-COVID conditions, one being long-haulers.”
Bagheri said in the beginning of seeing post-COVID patients, many health care providers did not believe them, or thought they wanted a letter for disability, until they realized that the post-COVID condition is a true condition.
“It was very vague,” he said. “Many patients complained about fatigue. They would say since they had COVID, they could no longer do the things they used to do, and many of those are young people. Interestingly, when they had COVID, it was not that severe. You could have a 30-year-old with COVID, that got a little sick, was never hospitalized, but never returned to base line, their normal life.”
Bagheri said the most common complaint is fatigue, tiredness, and lack of energy. But then other conditions began to surface. Many complained of “brain fog,” having difficulty thinking and concentrating. Many complained of headaches, fast heart rates, gastrointestinal symptoms, diarrhea, abdominal discomfort, loss of taste and smell, and lightheadedness and dizziness.
Bagheri said some people report mood swings, “just not the same person that they were before COVID.”
Bagheri said another longterm condition is a cough and shortness of breath, especially patients that were hospitalized, and developed COVID-19 pneumonia.
“This is a little different, and in these patients, the pneumonia can linger for a long time,” he said. “Even though they are not infectious anymore, months later their lungs are severely scarred with many of them having to be on oxygen for the rest of their life. They had pneumonia, low oxygen, and they never recovered with scarring and fibrosis in their lungs.”
He said another group of people, post-ICU syndrome, are patients that were extremely sick, ended up in the ICU, many on a respirator, had a long course of hospitalization, now suffer from weakness, difficulty concentrating, and posttraumatic stress disorder.
“When we talk about COVID patients, it is not just one patient population,” he said. “They could be young, elderly, healthy, have many preexisting medical conditions. And so is the severity of COVID. Many have minimal to no symptoms. Many get very sick and are in the hospital for a few months. The longer the length of hospitalization the longer the course of recovery.”
Bagheri said usually, most patients recover in one to six months, but there are still people 18 months later. Bagheri said they learned that it would take a multidisciplinary team to treat long haulers.
“Sharp Grossmont is the only Sharp facility and one of the few facilities in town that has a post COVID care clinic,” he said.
“For most patients, if they do not see a nutritionist, occupational therapist, specialists that are experts on their conditions, they may have a very slow recovery or may never get better,” said Bagheri. “That is why these post-COVID clinics are so necessary. Sometimes, just having someone to talk about their conditions with, and having that support system and groups is important, especially when people, even some care providers, do not believe them. This is such a new entity, so I think it is important that all health care providers need to understand that these conditions are real. Once that is taken seriously, then they need to do something about it.”
Bagheri said these clinics are now popping up across the country that include a multidisciplinary team of physical therapists, occupational therapists, speech therapists, vocational therapists, sleep experts, stress reduction experts like yoga and meditation, and other professionals that can focus on the many different post COVID problems.
“This multidisciplinary team is important,” he said. “That is why it is so important to open these types of clinics for post COVID conditions, and the multidisciplinary team can provide comprehensive and coordinated treatment for these patients, because no one person can treat these patients.”